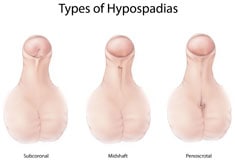
Overview: Hypospadias is an abnormality of anterior
urethral and penile development in which the urethral opening is anywhere along a line (the urethral groove) running from
the tip along the underside (ventral aspect) of the shaft to the junction of
the penis and scrotum or perineum. The
penis is more likely to have associated ventral shortening and curvature,
called chordee, with more proximal urethral defects.
Phenotype/Characteristics: The opening of
the urethra that carries the urine is located underside of the penis, and can
occur anywhere from just below the end of the penis to the scrotum. Hypospadias
can also manifest as an abnormally positioned genitals.
Severe hypospadias have associated
structural anomalies such as undescended testicles (10 % of cases) and inguinal
hernia. Enlarged prostaric utricle can predispose a patient to urinary tract
infections, pseudo-incontinence and stone formation.
This condition may cause a downward curve of the penis during
an erection. Erections are common in infant boys.
Other symptoms include:
- Abnormal spraying of urine
- Having to sit down to urinate
- Foreskin that makes the penis looks like it has a "hood"
Frequency: Hypospadias
occurs in up to 4 in 1,000 newborn boys. Sometimes, the condition
is passed down through families.
Diagnosis: This problem is almost always diagnosed soon
after birth during a physical exam. Imaging tests may be done to look
for other congenital defects.
The diagnosis of
hypospadias can be made prenatally using both prenatal fetal ultrasonography
and MRI.
Causes:
·
Genetic factors
o Inadequate human
chorionic gonadotropin (HCG) produced by a single placenta (commonly with
twins), with an inadequate supply during critical periods of urethral
development cause hypospadia
o Inhertitance is
polygenic; male children of fathers with hypospadias has been reported as 8%,
and 14% of brothers of children with hypospadias are also affected.
·
Endocrine factors
o A decrease in
available androgen or an inability to use available androgen appropriately may
result in hypospadias.
o A higher incidence of
hypospadias in winter conceptions has also been proposed.
o Other factors that
contribute to infertility, such as underlying endocrinopathies or fetal
endocrine abnormalities, may play a role.
·
Environmental factors
o Endocrine disruption
by environmental agents is blamed for increasing incidence
o Estrogenic substances
have been implicated in abnormal penile development in many animal models.
·
Combination theory: A growing body of
evidence suggests that the development of hypospadias is multifactorial
Treatment/Recommendations/Therapies:
Minor cases of
hypospadias, in which the meatus is located up toward the tip of the glans, may
not require surgical repair and may simply be managed with observation.
Infants with hypospadias
should not be circumcised. The foreskin should be kept for use in later
surgical repair.
Surgery is usually done
before the child starts school. Today, most urologists recommend repair before
the child is 18 months old. Surgery can be done as young as 4 months old.
During the surgery, the penis is straightened and the opening is corrected
using tissue grafts from the foreskin. The repair may require multiple
surgeries.
Because most
patients with hypospadias are surgically treated at a very young age, parental
teaching and reassurance is very important to ensure a satisfactory experience
for the families of patients with hypospadias. Evidence suggests that online
support groups can play an important role in how parents and patients cope with
this condition.
Support Groups:
Hypospadias and Epispadias Association,
Inc.
http://heainfo.org/
References:
Kaneshiro, N. (2012). Hypospadias. MedLine
Plus. Retrieved March 12, 2013 from the URL: http://www.nlm.nih.gov/medlineplus/ency/article/001286.htm
Gatti, J. (2011). Hypospadias. MedScape.
Retrieved March 12, 2013 from the URL: http://emedicine.medscape.com/article/1015227-followup#a2651
Photo from:
http://www.cdc.gov/ncbddd/birthdefects/images/hypospadias-sm.jpg
Photo from:
http://www.cdc.gov/ncbddd/birthdefects/images/hypospadias-sm.jpg

Walang komento:
Mag-post ng isang Komento